Aortic Valve Surgery
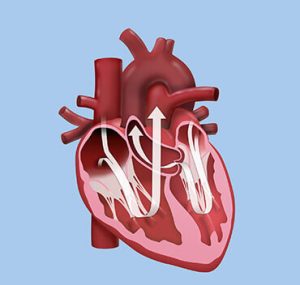 The Aortic Valve is the outflow valve from the main pumping chamber (left ventricle) and is not uncommonly affected by progressive fibrosis and calcification as part of the aging process. This can cause the valve to obstruct the flow of blood out of the heart causing increased work for the left ventricle, this is called “Aortic Stenosis”. As it progresses symptoms of tiredness and shortness of breath can develop. This condition can also occur when the valve is abnormal from birth. This is called a “Bicuspid” aortic valve and occurs when the normal 3 leaflets of the valve do not separate properly, leaving 2 leaflets instead. This type of valve tends to become obstructive much earlier, often in the 40-60 year age group. Untreated it can lead to premature death.
The Aortic Valve is the outflow valve from the main pumping chamber (left ventricle) and is not uncommonly affected by progressive fibrosis and calcification as part of the aging process. This can cause the valve to obstruct the flow of blood out of the heart causing increased work for the left ventricle, this is called “Aortic Stenosis”. As it progresses symptoms of tiredness and shortness of breath can develop. This condition can also occur when the valve is abnormal from birth. This is called a “Bicuspid” aortic valve and occurs when the normal 3 leaflets of the valve do not separate properly, leaving 2 leaflets instead. This type of valve tends to become obstructive much earlier, often in the 40-60 year age group. Untreated it can lead to premature death.
Aortic stenosis has been well managed with Aortic Valve Replacement (AVR) for many years. This can be performed using a “mechanical” valve (made of carbon), or a “tissue” valve (made from a pig’s valve or cow’s heart lining). Both work well, the difference being that the mechanical valve requires lifelong anti-coagulation (Warfarin) whilst the tissue valve does not, but tissue valves can wear out after 10-20 years. Tissue valves last longer the older the age at surgery, such that after 65 there is very little chance of the need for another surgery because of the valve wearing out. The valve selection is an important discussion that must occur between patient and surgeon. Each patient has individual features that determine which valve best suits their needs.
The surgery is traditionally performed via a sternotomy incision, and is done this way if other surgeries are needed at the same time. Minimally invasive techniques are now available for performing isolated AVR. This is done using a 6-8cm incision over the right chest wall, with no need to split the breast bone. This speeds up the recovery period allowing earlier return to full activity.
Replacement options have recently increased with the introduction of “TAVI” or Trans-catheter Aortic Valve Implant. This technique uses traditional tissue valve leaflets mounted on a collapsible metal frame that is then delivered by catheter across the aortic valve and re-expanded, creating a functioning valve. There is no need for stopping the heart and most are inserted via a small incision in the groin. The diseased valve is left in place and simply pushed aside by the new valve. Whilst this has some benefits it also has a few problems, for this reason this procedure is currently best utilised in those at a higher risk from undergoing conventional AVR. This would be part of the discussion your cardiologist and surgeon would have prior to suggesting your surgery.
Conventional, Minimally Invasive, and TAVI are all available through this practice. The aortic valve can also be affected by Leaflet weakening, Rheumatic Fever, Aortic Root Aneurysms, or Infections, all of which cause the valve to leak or “Aortic Incompetence”. This requires surgical intervention when it becomes severe enough to cause symptoms or affect the left ventricle function. This usually requires the valve to be replaced, though some conditions are able to be repaired.